Gastrointestinal surgery is a treatment for diseases of the parts of the body involved in digestion.
Gastrointestinal surgery is a treatment for diseases of the parts of the body involved in digestion. This includes the esophagus (food pipe), stomach, small intestine, large intestine, and rectum. It also includes organs like the liver, gallbladder, and pancreas.
Surgery may be used to remove any growth or damaged part of the body, such as the intestine. It may also be used to rectify a problem like a hernia (a hole or weak spot in the wall of the abdomen). Minor gastrointestinal surgical procedures are used to screen and diagnose problems of the digestive system.
Gastrointestinal surgery is done by taking incisions into the abdomen with a scalpel (a surgical knife) and other tools. Some surgery is done with a scope — a thin tube with a camera and small surgery tools.
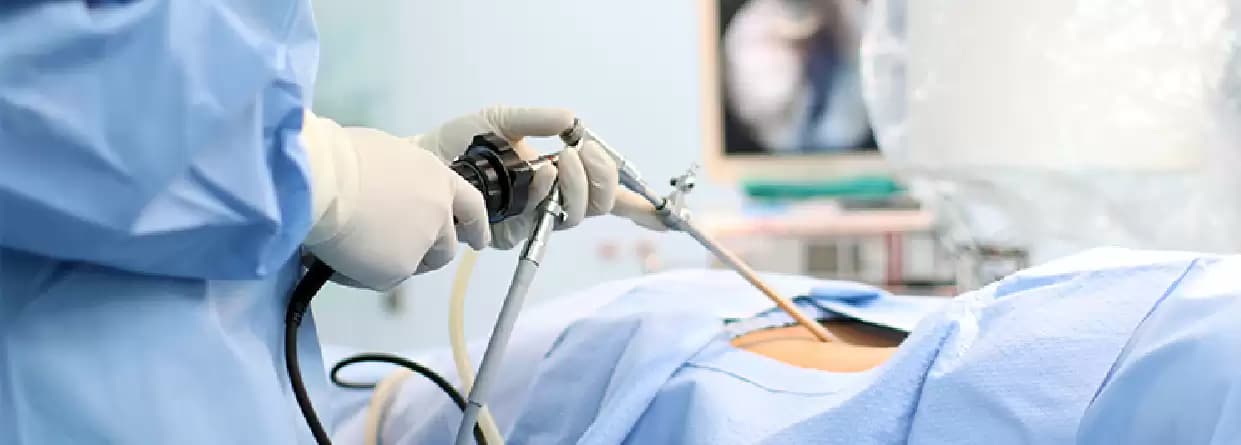
Laparoscopic surgery and hand-assisted laparoscopic surgery (HALS) are “minimally invasive” procedures commonly used to treat diseases of the gastrointestinal tract. Unlike traditional surgery on the colon or other parts of the intestines where a long incision down the center of the abdomen is required, laparoscopic surgery requires only small “keyhole” incisions in the abdomen. In the case of hand-assisted surgery, a 3 to 4-inch incision is also used to allow the surgeon’s hand access to the abdominal organs. As a result, the person undergoing the procedure may experience less pain and scarring after surgery and a more rapid recovery.
During Gastrointestinal laparoscopic surgery, ideally three or more small (5-10 mm) incisions are made in the abdomen to allow access ports to be inserted. The laparoscope and surgical instruments are inserted through these ports. The surgeon then uses the laparoscope, which transmits a picture of the abdominal organs on a video monitor, allowing the operation to be performed.
Before laparoscopic surgery is scheduled, your surgeon will take a detailed history and do a thorough evaluation and examination. Your intestine will require cleaning and you will be given a prescription for a laxative medicine to take the evening before the surgery.
All patients are generally asked to provide a blood sample. Depending on your age and general health, you may also have an ECG (electrocardiogram), a chest X-ray, lung function tests, or other tests.
Finally, you will meet with an anesthesiologist, who will discuss the type of pain medication (anesthesia) you will be given for surgery, and you will learn about pain control after the operation.
The evening before surgery you will need to take the prescribed laxative medicine. It is important to follow the directions carefully and drink all of the laxatives. This step will decrease your risk of developing an infection from bacteria normally present in the intestine.
Food and any other drinks by mouth is prohibited after midnight or the evening before surgery.
Post-operative the patients are kept on assisted respiration and intubated. Pain medication will be given as per the progress of recovery. It is important to document all the intake of and measure and collect any liquid outputs, like urine, and also include those from tubes or drains placed during the operation.
Nausea and vomiting happen in approximately 5%-10% of people and occur because your intestines are temporarily disabled from the operation. In addition, anesthesia makes many people nauseous. For this reason, food and drink are given slowly for the first few days.
You will be encouraged to get out of bed and walk, starting the first day after the operation. The length of your hospital stay will depend on the type of procedure you have and how quickly you recover.
Written and Verified by:

Dr. Anukriti Sood is a Consultant Breast & Endocrine Surgeon at CK Birla Hospital, Jaipur, with over 6 years of experience. She specializes in breast surgery (benign and malignant), thyroid and parathyroid disorders, and women's health awareness.
Similar General Surgery Blogs
Book Your Appointment TODAY
© 2024 RBH Jaipur. All Rights Reserved.